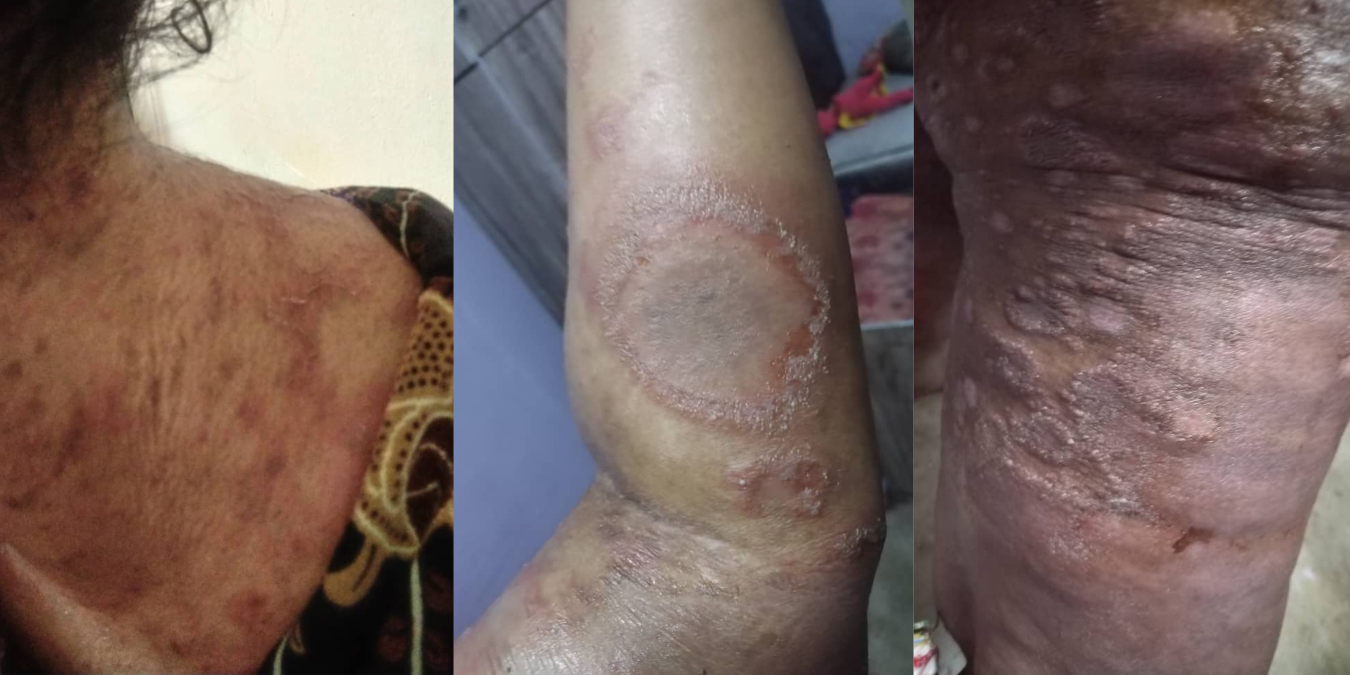
KUALA LUMPUR, Nov 21 – Kristina Siranjivi was 17 years old back in 2011 when she suffered from itchy, scaly patches on her scalp, knees and elbows. The condition would flare up for a few weeks, and then subside for a while.
She was put on antibiotics to treat any possible infections, but it was later discovered that the antibiotics were a triggering factor that caused her condition to flare up.
Kristina, who is now 31 years old, said she was diagnosed with plaque psoriasis, a condition she says runs in her family, as her aunt, uncle, and niece have also suffered from it.
“At that time, it was really difficult for me to understand what was happening with my body,” she told Ova in an email interview. “The plaque psoriasis required a lot of time to manage and control. As a result, I struggled to focus on my studies, and my plans for further education suffered.”
Things took a turn for the worse a few years later in 2019 when her whole body became covered in pus-filled blisters. Kristina was immediately hospitalised and put on intravenous (IV) antibiotics and steroids to reduce the inflammation.
“When I was hospitalised in 2019, I underwent several blood tests which revealed that there was an infection in my system, but the doctors were unsure what was causing it,” she said.
“Fortunately, they persisted in running more tests, and one week later, it was confirmed that I was suffering from Generalised Pustular Psoriasis (GPP).
Difference Between Plaque Psoriasis And Generalised Pustular Psoriasis

GPP is a rare and severe form of psoriasis, according to Dr Azura Mohd Affandi, a consultant dermatologist at Hospital Kuala Lumpur (HKL).
She explained to Ova in an email interview that it is a chronic and potentially life-threatening disease characterised by primary, sterile, and macroscopically visible pustules.
Pustules are small raised areas on the skin that contain pus.
GPP is distinct from plaque psoriasis in many ways, said Dr Azura. “It is considered a neutrophilic autoinflammatory disease, a condition characterised by an abnormal number of neutrophils (a type of white blood cell involved in fighting infections), whereas plaque psoriasis is considered an autoimmune disease, where the immune system mistakenly attacks and damages the body’s own tissues, instead of protecting it.”
She said the diseases also differed in both appearance and severity. “While plaque psoriasis presents with raised, red patches covered in silvery scales, GPP is characterised by widespread pustules filled with non-infectious pus on inflamed, red skin.”
Plaque psoriasis is typically a chronic condition with slower progression and fewer acute, life-threatening symptoms, but GPP can cause systemic symptoms such as fever, chills, and fatigue, making it a medical emergency in severe cases, according to Dr Azura.
Whole Body Covered In Pus-filled Blisters
When she experiences a flare, Kristina said her skin usually turns very red with oozing, pus-filled bumps all over the body, even on the soles and sides of her feet, causing a burning and itching sensation.
“It is nearly impossible for me to perform daily tasks without help. I struggle with balance and often feel dizzy, which can make walking even inside my home, such as to the bathroom, challenging, and putting me at risk of falling.
“Bending down to pick up items or perform household chores feels physically exhausting, as I also suffer from joint stiffness and body aches due to the inflammation of my joints.”
When she was initially hospitalised for GPP in 2019, Kristina was treated with antibiotics, topical steroids and an immunosuppressant.
“However, I developed seizures as a side effect from the medication. The initial seizure was so violent that I fell in the bathroom and hurt my head,” she told Ova.
“It also caused me to fall out of bed several times. Following this, I was taken off the immunosuppressant and prescribed other medications to control the pus-filled blisters on my skin.
“Unfortunately, these medications caused me to lose my hair in clumps to the extent that my scalp was nearly visible, while causing facial acne and an alarming spike in my blood cholesterol levels.”
As she was unable to tolerate the treatments, Kristina was put primarily on antibiotics and steroids to manage her GPP flares while she was in the hospital. The medicines are delivered through intravenous (IV) drips to stop the reaction quickly.
The flares typically subside within two to three days upon the administration of the IV treatments. After she is discharged from the hospital, she is usually prescribed steroids.
“I have noticed my GPP flares are triggered by several things, such as migraines or toothaches, and particularly, the hormonal fluctuations that occur during my menses,” Kristina said.
“My flare usually lasts about three months each time, including at least two weeks of hospitalisation, before it subsides and my new skin forms.
“However, this relief is short-lived, as my next menses will almost certainly trigger another flare! In other words, I have to manage my GPP flares nearly all year round.”
Kristina has to travel repeatedly from Subang Jaya (where she lives) to Hospital Kuala Lumpur, which is about 30 minutes away if traffic is smooth, to receive treatments, “The trip to hospital can be exhausting and time-consuming,” she said.
In fact, she was just hospitalised for a flare recently. This time she was administered a newly-approved intravenous (IV) treatment called interleukin-36 receptor (IL-36R ) inhibitor to reduce and control the severity of her flares.
Within just one day of receiving the treatment, the pus-filled blisters on her skin started to subside and dry out. The flares receded within the next three days.
“My skin no longer felt raw,” she said. “I was discharged after just three days, unlike in the past when I would be hospitalised for at least two weeks. Best of all, I did not suffer any side effects.”
Pharmacological Treatment Protocols For GPP
Pharmacological treatment protocols for GPP flares prioritise stopping the formation of pustules and reducing skin redness, Dr Azura told Ova.
“Immediate medical intervention is crucial during flare-ups, as untreated severe cases can become life-threatening.”
The management of GPP is based on the severity of the flare, categorised into mild, moderate, and severe levels. Treatment typically starts with topical steroids for mild flares.
If the treatment is ineffective, patients would be prescribed non-biologic treatments such as acitretin, cyclosporine, or methotrexate, according to Dr Azura.
For moderate flares, non-biologics such as acitretin, cyclosporine, or methotrexate are recommended.
“Once symptoms such as fever, pustules and skin issues improve, the patient moves on to maintenance protocols, with lower doses of the mentioned drugs,” Dr Azura said.
In severe cases like Kristina’s, fast acting biologics such as the IL-36R inhibitor are required. The IL-36R inhibitor was approved by the United States’ Food and Drug Administration (FDA) in September 2022 specifically to treat GPP flares in adults, according to Dr Azura.
She added that it was approved for the treatment of GPP flares in Malaysia in October this year. If biologics are unavailable, high doses of acitretin or cyclosporine are used.
Awareness Of GPP Among Health Care Professionals Crucial

“If generalised GPP is left untreated, it can cause life-threatening complications such as renal complications, hepatic complications and cardiac complications,” Dr Azura said.
“The open sores from the skin lesions can also increase the risk of infections, which may trigger systemic inflammation, further exacerbating cardiac issues.”
One of the critical challenges in managing GPP is the lack of awareness about the condition and its symptoms, among primary care physicians, she told Ova, adding that GPP is often misdiagnosed as a bacterial, fungal, or severe systemic infection like sepsis.
As a result, many patients with GPP might be treated for infections, which could exacerbate their condition and delay appropriate treatment.
“Early recognition is crucial because it reduces the risk of inappropriate treatment, such as antibiotics, which do not address the underlying issue, and allows for faster, more effective interventions that can significantly improve patient outcomes,” Dr Azura said.
She added that it is important to raise awareness about GPP among health care professionals.
“It is crucial for general practitioners (GPs) and emergency department doctors to be trained to recognise the symptoms and distinct features of GPP so they can refer patients to a dermatologist promptly.”
As some symptoms of GPP can mimic other autoimmune diseases, it is vital that specialists perform the relevant tests to identify GPP as early as possible, she continued.
“Delays in diagnosis and treatment can worsen outcomes for the patient and increase the risk of severe, life-threatening complications.”
Although it is relatively rare, awareness of GPP is crucial because it represents one of the most severe forms of psoriasis, Dr Azura said.
According to the Twelfth Report of the Malaysian Psoriasis Registry, only 1.6 per cent of total patients with psoriasis report GPP, but its impact is profound and can be life-threatening.
Between 2010 and 2020, 230 people were estimated to be living with GPP in a Malaysian population of 1.1 million, which means that the prevalence of GPP in Malaysia is 198 per million individuals, which accounts for approximately 0.02 per cent of the population.
The condition appears to be more prevalent among females with a particularly high incidence among the Chinese ethnic group, compared to Indians and Malays.
GPP can appear in any age group, although is most common in adults between 40 to 50 years old.
“The age of onset is often earlier in patients with a family history of psoriasis, or with gene mutations, such as the interleukin receptor antagonist (IL36RN) gene mutation among others,” Dr Azura said.
It can also affect pregnant women, which is termed impetigo herpetiformis, and is associated with increased maternal and foetal morbidity.
GPP Significantly Impacts Daily Activities, Quality Of Life

Dr Azura said it is just as important to raise awareness about GPP among the public. “Patients with GPP are often subjected to stigma or discrimination due to the visible and unpredictable nature of their flares.
“Sometimes they require prolonged hospital stays because of the flares and this also causes them to take leave from work for an extended period of time.
“It is crucial that colleagues and supervisors support and have understanding and empathy for individuals living with chronic conditions like GPP,” she added.
“We hope that reducing the stigma around this condition will help to improve the quality of life for GPP patients.”
In April this year, Kristina, who was a business administrator, made the difficult decision to resign from her job due to frequent hospitalisations and medical leave as a result of GPP.
“Having to pay for medical treatments and hospital visits, and the loss of income from my resignation have put my family in a difficult financial situation,” she told Ova.
While her regular hospital visits only cost RM5 per visit at the government hospital, frequent hospitalisation can incur additional charges of up to RM280 per admission.
She also has to fork out money for certain medications such as coal tar shampoo, petroleum jelly ointments, and fungal creams.
“Although covered by the government, it is limited in supply, so I usually need to purchase them out of pocket from the private pharmacy,” she said.
“At times, my doctor may also prescribe certain medications such as corticosteroid shampoos which are only available from the pharmacy.”
Kristina also struggles with juggling family responsibilities such as looking after her two children and undergoing treatments for GPP as prescribed by her doctors.
“For example, I was previously required to go to the hospital three times a week, to undergo ultraviolet (UV) treatment for plaque psoriasis, but I was unable to do so because I had to take my children to school and handle other family commitments.”
She said the disease has significantly impacted her daily activities and quality of life, as she does not know when her flares will erupt and how severe each episode will be.
“I feel frustrated and helpless very often as I am unwell and unable to carry out daily tasks. I have to live with visible scars all over my body, even when I am not having a flare,” Kristina said.
“My social life has been severely affected, as I prefer to isolate myself than to explain my skin condition to those whom I don’t know well.”
She told Ova when her condition felt too unbearable before, she considered taking her own life. However, thoughts of her late grandmother, who had raised her, held her back.
“She always lifted me up when I was feeling down and gave me emotional support to carry on at the worst times in my life.”
The Healing Kit

Patients with GPP endure extreme pain due to the inflammation and pustules covering their skin, said Dr Azura.
“Their entire skin surface can become so inflamed that even basic movements, such as raising a hand or getting out of bed, become excruciatingly difficult and painful.
“The fluid-filled pustules can also burst and cause the skin to stick to the clothing and bed sheets, leading to additional pain and abrasion on the skin when they attempt to move.”
She added that even showering can be distressing for GPP patients as water on inflamed skin can cause intense pain.
“One of the complaints we often hear from patients with active GPP flares is that the conventional hospital gowns tend to irritate or aggravate their skin, and many patients prefer to not wear any clothes during their stay.”
To address this issue, The Healing Kit was developed through a collaboration between the Psoriasis Association of Malaysia (PAM), Boehringer Ingelheim, and Oxwhite®.
Items in The Healing Kit include hospital gowns and towels made from soft, breathable fabric that reduces skin irritation and is suitable for hot and humid climates.
It also includes a toothbrush with soft bristles that is meant to be gentle on inflamed gums. Additionally, it contains a journal to help patients monitor and track their symptoms and flares, so they can manage their disease better.
“My focus when developing The Healing Kit was primarily on the functionality and comfort of the items, more than aesthetics,” Dr Azura said.
“We also hope the items in The Healing Kit can offer some comfort and relief to patients while they are waiting for their medications to take effect.”
She said GPP patients should adopt lifestyle modifications and supportive therapies as part of the non-pharmacological management of GPP.
These may include stress management techniques, practising a healthy balanced diet, sufficient rest and maintaining skin hydration.
Patients are also advised to avoid known triggers such as stress, infections, and extreme weather conditions.
Additionally, support groups and counselling can also aid them in coping with the emotional burden of the disease.
Kristina’s Advice

Kristina said she is lucky that her husband, who is now the sole breadwinner, and her siblings are very supportive, attending to her needs and helping with the household chores and care of her children.
“My advice to others suffering from this condition, is to be patient and allow yourself time to adjust to this diagnosis. The journey with GPP is very difficult, but your mindset can make all the difference,” she said.
“Learn to accept your condition and trust that, over time, you will find ways to manage it.”
She added that those who suffer from GPP should not be afraid to say ‘no’ to unwanted or unsolicited advice, and set firm boundaries to reduce their stress.
Kristina said she has found some help and relief by following some social media pages, such as the psoriasis patients’ group in Hospital Kuala Lumpur, where patients share their stories on living with and managing GPP.
“While I do not actively participate in any support groups, it is helpful to hear/ see others’ experience with similar struggles,” she said.
“I think sometimes life’s challenges are meant to show us how much strength we have. Hold on to that strength, and take it one day at a time.”