KUALA LUMPUR, April 13 — As the sole rehabilitation physician serving patients in Kuala Pilah and Jempol, Negeri Sembilan – where the population combined is almost 200,000 – Dr Intan Sabrina Mohamad has to rely on telemedicine to provide her services.
In the past year, she has tended to the stroke rehabilitation needs of communities in rural areas that are populated mostly by indigenous people and the elderly.
She shares that way of life, less sophisticated devices and technology, and language are among the challenges she faced in ensuring that patients get the care they need.
“In many rural areas, elderly couples only have Nokia phones, not even smartphones. They live with their children and grandchildren, so one device is usually shared between two to five people,” said Dr Intan, who is a rehabilitation physician with Tuanku Ampuan Najihah Hospital, Kuala Pilah; Jempol Hospital, Bandar Seri Jempol; and Tung Shin Hospital, Kuala Lumpur.
With the onset of the Covid-19 pandemic, a lot of schoolchildren in these areas had to undergo learning from home, complicating matters in terms of access to devices and scheduling of sessions.
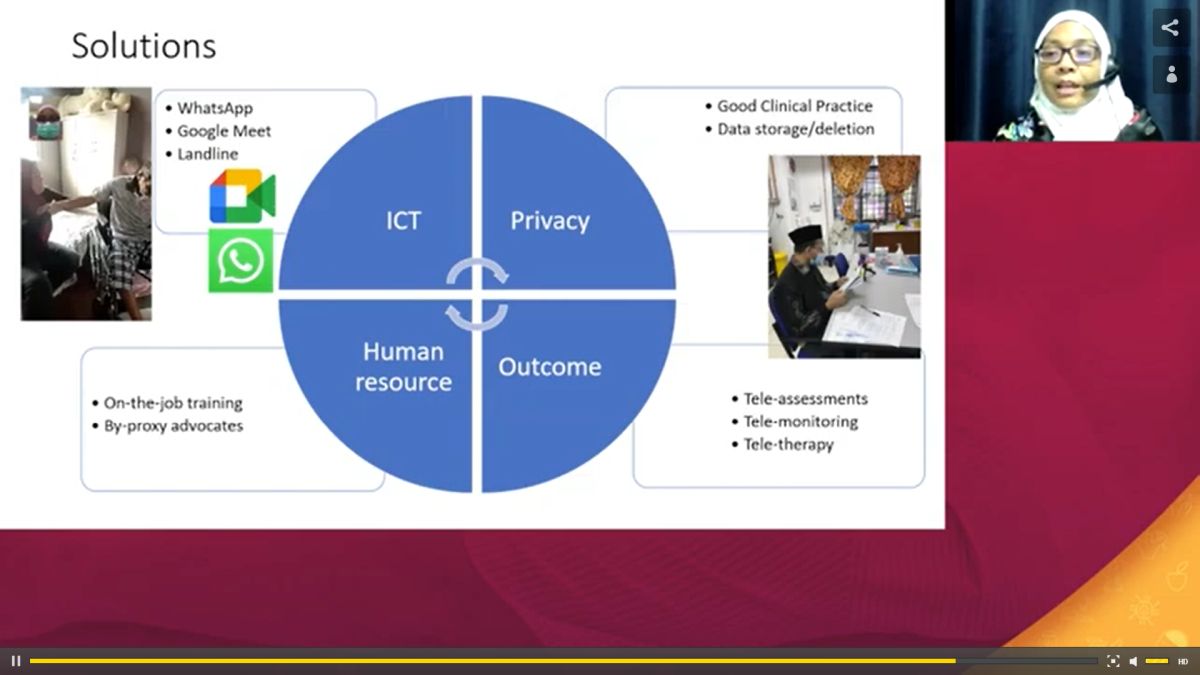
“It’s challenging for our rehabilitation team to provide care. It needs to be planned beforehand,” she said during her presentation on “Telemedicine – Delivering Health Care in Rural Areas” at the 10th Hybrid Conference on Healthy Ageing held from March 15 to 17.
Despite calling patients on landlines and texting them to remind them of their pre-scheduled appointments, patients still tend to forget their appointments.
“They will say ‘yes, we’ll be there’, but they don’t quite understand what teleconsultation is. So it takes a few rounds for us to educate and train them on telemedicine and all its components.”
Teleconsultation sometimes takes place at inconvenient locations, such as paddy fields, where poor connectivity may interfere with the session.
There have also been instances when patients were at their verandahs during consultation and the sound of motorcycles could be heard roaring in the background.
She said that patients had to be educated on the need to dedicate a quiet room or space for their teleconsultation sessions.
“We have to tell them that your grandchildren need to be confined in a certain area of the house and not be running around crying and screaming.”
Since one device is shared by up to five people, privacy also becomes an issue.
“Especially confidentiality which is quite challenging to observe,” said Dr Intan. “When it comes to areas like sexual related issues and infections, we have to be mindful of how we go about it.”
Communication can also pose a problem as she encountered language barriers and patients who were illiterate.
“The pandemic has exposed us to pockets of communities who do not speak Bahasa Melayu or even English,” she said.
“They can’t read or write so we would have to employ advocates for them such as their neighbours or the nearest Klinik Kesihatan doctors or nurses. Sometimes, the Klinik Desa nurses or medical assistants have to go to their houses and facilitate the teleconsultation.”
Occasionally, she would employ the assistance of medical officers and therapists to provide recorded demonstrations for the patients. Similarly, patients are asked to record their activities such as bathing, eating, and exercise to send to medical staff.
“So, it’s been an on-the-job training for both parties, the caregivers as well as our staff, on how to conduct teletherapy and go beyond just consultation,” said Dr Intan.
Hybrid Care Model: Online And Offline

According to Dr Raymond Choy, CEO and co-founder of DOC2US, an online health care consultation service, the adoption of telemedicine skyrocketed during the pandemic. Downloads for medical apps grew by 50 per cent year-to-year due to Covid-19.
“Private hospitals rolled out telemedicine in four weeks. Usually, it takes them about four to five years. So you can see there was a trigger, there was a pain. Change is painful but hospitals had no choice but to pivot and evolve,” he said.
“Some doctors may argue I prefer working offline because that’s the way I was trained. But the pandemic has proven the value of digital health. If we keep practising offline, it won’t be relevant to today or tomorrow’s health care needs.”
However, he maintained that health care is not a field that can go completely digital because it requires human touch and demonstration of empathy, which are difficult to deliver in a virtual setting.
“The threshold for referrals in virtual consultations are much lower compared to physical consultations,” he said. “We believe a hybrid care model should be the way where online and offline complement each other.”
Dr Choy said health care providers should also consider the costs of treatment for their patients to ensure sustainability in the long run. “If we prescribe branded drugs and patients can’t afford them, they won’t be able to sustain.
“We have to think about the socioeconomic status of patients and how we can make it better and cheaper for them but provide the same outcome.”
Costs are an important factor in the health equation, he said, adding that implementation of digital health care nationwide should be targeted for people from all walks of life.
“Health care should be inclusive, not exclusive, and is accessible to all.”
Digital health care provides health professionals with the opportunity to extend their services to patients in the outskirts and in rural areas, provided the infrastructure can accommodate it.
“Rural areas – if the infrastructure is not ready, don’t talk about high technology,” said Dr Choy.
“Digital health is not really about high tech, it’s about how you can provide value to people, using technology.
“You don’t necessarily need to do a virtual consult or use video or whatever. You can use SMS to remind patients to take their medicine, to remind patients to take their blood glucose.
“That works especially for certain B40 (bottom 40 per cent) groups. And they are very SMS driven, so we have to understand the behaviour of our patients and consumers.”